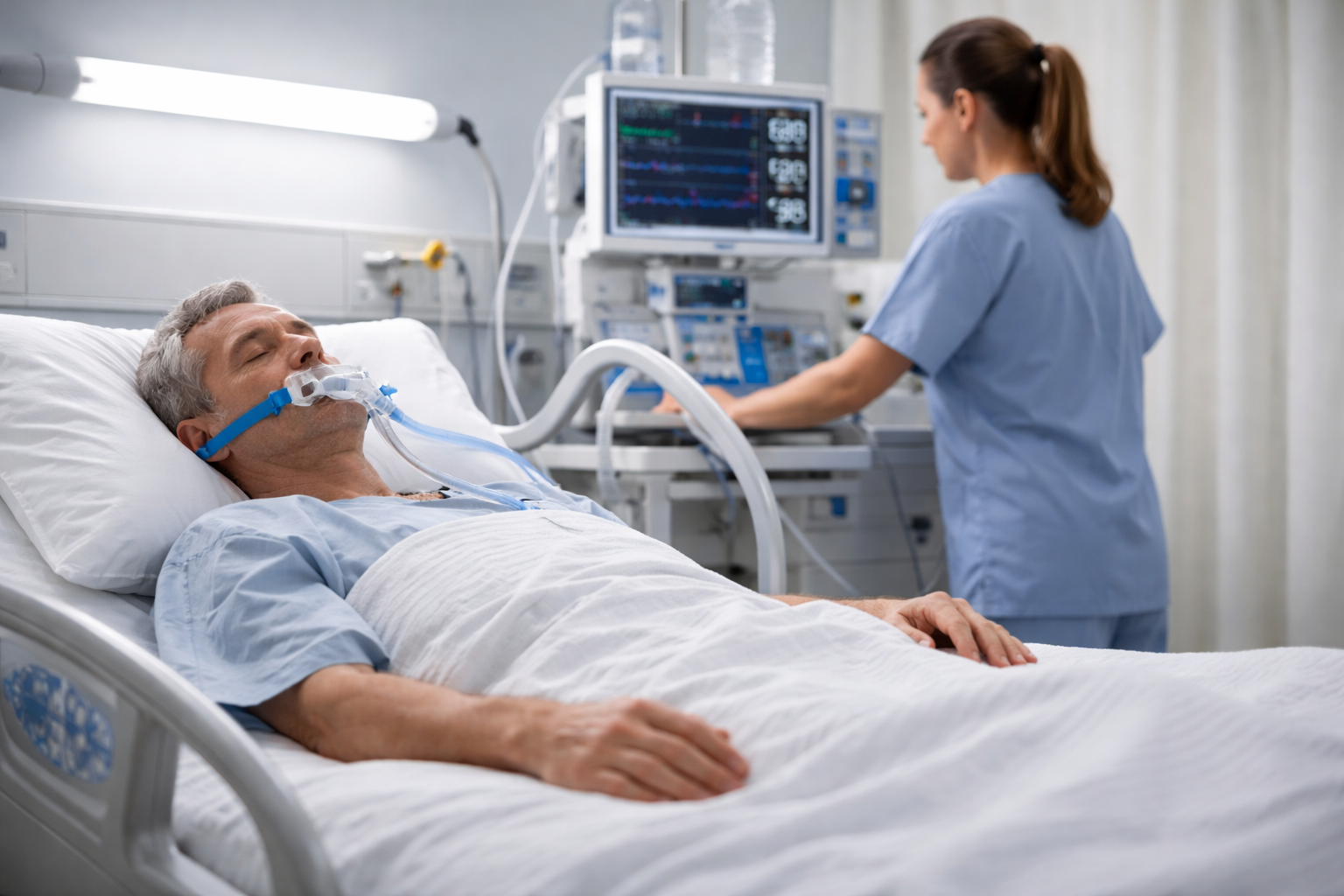
Doctors Rethink Use of Restraints for Patients on Ventilators
A new medical trial has made people very worried about the common use of physical restraints on people who are on breathing machines, or ventilators. For a long time, doctors and nurses thought that keeping patients from moving around would keep them from getting confused, pulling out their breathing tubes, or hurting themselves. But this new study shows that these restraints might not be as helpful as people thought, and they might even do more harm than good.
This is an important discovery because every day, thousands of people around the world are put on ventilators, mostly in intensive care units (ICUs). To improve care and save lives, it is important to know what really helps these patients get better safely.
Why Physical Restraints Were Commonly Used
Physical restraints are things or ways to keep a patient from moving around. These can be things like wrist straps, belts, or special beds. They are often used on patients who are unconscious, confused, or can’t control their actions.
The main idea behind restraints was simple: if a patient can’t move around freely, they’re less likely to accidentally pull out important medical tubes, like the one that helps them breathe. It was also thought that restraints could help ICU patients who are delirious, which is a medical term for being confused.
But the new trial showed that this method doesn’t work as planned. Patients who were restrained were not less likely to be confused. They were just as likely to go crazy as people who weren’t restrained. Also, using restraints didn’t make it less likely that patients would pull out their breathing tubes.
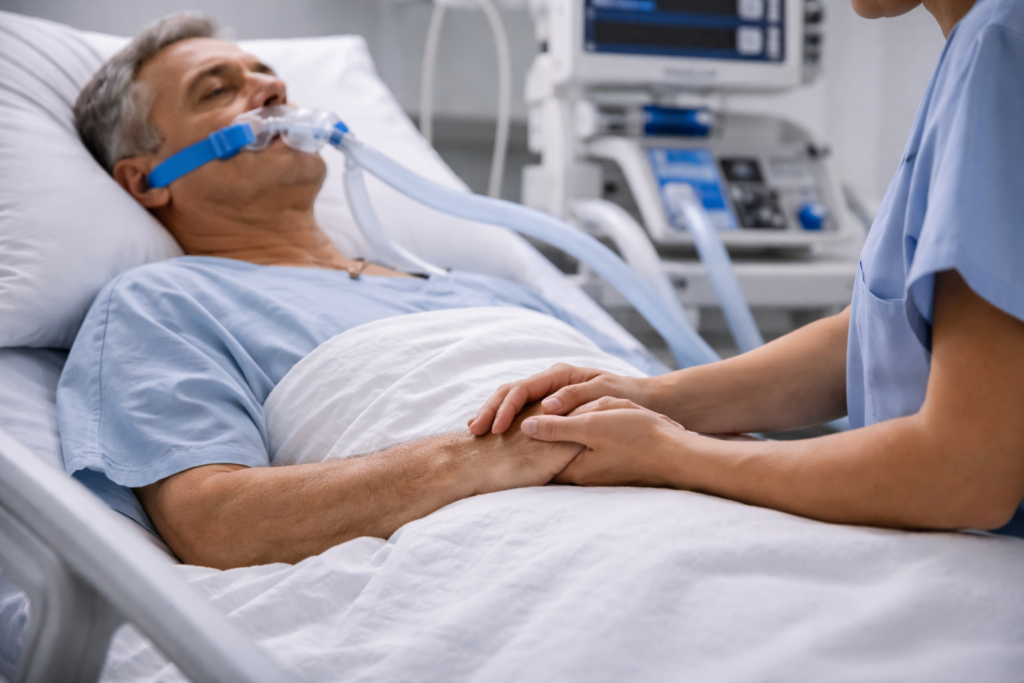
The study also showed that restraints did not lower the number of deaths, which was even more surprising. This goes against what critical care medicine has believed for a long time and suggests that using restraints all the time may not be helpful at all.
What This Means for the Care of Patients
These results are making doctors and nurses rethink how they care for patients who are on ventilators. Many hospitals are now focusing on safer and more humane alternatives to restraints instead of using them.
Better monitoring of patients is one important way to do this. Nurses can watch over patients more closely and act quickly if they show signs of distress or confusion. Another way is to make communication better, even with patients who can’t talk. Simple things like explaining procedures, keeping the environment calm, and including family members can help ease anxiety and confusion.
People are also looking at how sedation is done. Too much sedation can make people more confused, and too little can make them restless. Finding the right balance is important for keeping patients safe and comfortable.
Another trend that is growing is early mobility. When you can, helping patients move, sit up, or even take small steps can help them get better and lower their delirium. It may sound strange, but moving around gently can actually help the brain stay awake.
Overall, this new study shows how important it is to put the patient first in care. It reminds us that not all old ways of doing things work, and some may need to change when new evidence comes to light.
In summary, using physical restraints on patients who are on breathing machines on a regular basis does not seem to help with confusion, stop tube removal, or save lives. Because of this, healthcare providers are being urged to use safer, more helpful methods. This change could lead to better outcomes, more comfort for patients, and a higher standard of care in hospitals all over the world.